Physician Development: Growth Never Stops
Physician Development: Growth Never Stops
It was a hot August day. I walked into my first day of medical school orientation wearing shorts and a T-shirt, flanked by two roommates. One roommate I had known through all of undergrad, the other I met just a few days before through an old-fashioned “roommate needed” posting on a bulletin board.
As I looked around the room, I could not believe I was there.
I was convinced someone was going to figure out I did not belong. That the dean would call me into his office and say, “We made a mistake in the admissions process. There is someone smarter than you who should have your spot, and classes start Monday.”
I also thought I was the only one who felt that way.
I was not.
What nobody told me that August — and what I have spent much of my career trying to tell others — is that the self-doubt you feel at the beginning of any new chapter in medicine is not evidence that you do not belong. It is evidence that you are paying attention. You understand the weight of what you are stepping into. It means you care.
And here is what I have learned across more than two decades in medicine, as a clinician, educator, fellowship director, and coach: that cycle never fully disappears. The doubt returns at every new threshold. What changes is your relationship to it.
The direct answer: Physician development is a lifelong process, not a destination. From premed to division chief, every career stage involves a predictable cycle of doubt, growth, adaptation, and emerging confidence. Understanding that cycle — and having a framework for navigating it — is the difference between thriving in medicine and surviving it. This page is your starting point.
Why Physician Development Matters Beyond Training
Medicine prepares us extraordinarily well for one thing: clinical care. We learn to diagnose, treat, and manage. We develop clinical reasoning through years of supervised experience. By the time we finish training, we know how to care for patients.
What medicine rarely prepares us for is everything else.
How to lead a team or navigate an institutional conflict. Mentoring a struggling resident. Setting boundaries with an administrator without torching the relationship. How to sustain yourself across a 35-year career without losing the person you were when you started.
These are not soft skills. They are the infrastructure of a sustainable career in medicine. And they develop — like clinical skills — through deliberate practice, feedback, and reflection.
The field of adult learning has known this for decades. Medicine is only now catching up.
For the full framework on burnout and what happens when physician development stalls: Physician Burnout, Moral Injury & Ordinary Joy.
Resources on physician leadership development and mentorship: Physician Leadership & Mentorship.
About career growth and nonclinical paths when medicine needs redesigning: Physician Career Growth & Nonclinical Paths.
What Adult Learning Theory Teaches Us About Physician Growth
In 1968, Malcolm Knowles introduced the concept of andragogy — the art and science of helping adults learn — and distinguished it sharply from the pedagogy used to educate children. Children learn because they are told to. Adults learn because they need to. They bring prior experience and are self-directed. Adult learners want to know why something matters before they invest in learning it. They learn best when the content connects immediately to real problems they are facing.
Sound familiar? It should. Every physician in a difficult call night, a hard family meeting, or an unexpected leadership challenge is learning — not because a curriculum told them to, but because the situation demanded it.
Knowles’ principles map almost exactly onto what I have seen in two decades of physician coaching:
- Adults are self-directed learners. Physicians resist being told what to do. They respond to frameworks that help them see what they want to do next. Coaching works not because a coach prescribes a path, but because the process surfaces what the physician already knows and helps them act on it.
- Adult learning is experience-based. What shapes a physician is not the lecture but the patient — the case that did not go as expected, the feedback that landed hard, the mentor who saw something you could not see yet. Experience without reflection, however, is just accumulated time. Reflection is what transforms experience into growth.
- Adults learn when they see relevance. Tell a junior attending they need to develop leadership skills and you will get a polite nod. Show them how those skills will help them protect their team, navigate their next promotion, or reclaim 45 minutes per day — and they lean in.
Building on Knowles, Jack Mezirow’s transformative learning theory adds another dimension critical to physician development: the idea that the most profound growth happens not when we acquire new information, but when we examine and revise the assumptions that shape how we see ourselves and our work.
The physician who has spent a decade believing that working harder is always the right response is not going to change that pattern by reading an article about work-life balance. The pattern shifts when something disrupts the assumption itself — a coach who asks the right question, a health scare, a colleague who models something different — and the physician begins to examine whether the assumption still serves them.
This is exactly what I try to create in coaching: not advice, but perspective shifts.
David Kolb’s experiential learning cycle completes the picture. Kolb proposed that learning moves through four stages: concrete experience, reflective observation, abstract conceptualization, and active experimentation. In medical training, we give physicians enormous amounts of concrete experience. We are not equally deliberate about reflection, conceptualization, or creating safe space for experimentation. The result is a workforce that accumulates experience rapidly but sometimes struggles to extract and apply the lessons from it.
The Developing Doctor Evolution Ladder draws on all three of these traditions. It is not a checklist. It is a developmental map.
Two Swimmers at the Pool: Why Competence and Professionalism Are Separate Tracks
Before I get to the Evolution Ladder itself, I want to explain the insight that shaped how I think about physician development. It came not from a textbook but from a pool.
I started swimming competitively when I was six years old. I swam through childhood, competed in master swimming as an adult, and spent years as a lifeguard and swimming instructor — through high school, college, and into medical school. Swimming taught me things about development that no course on adult learning ever did.
Here is the lesson that stuck with me most.
One of the pools I worked at had a standard rule: anyone new to the facility had to demonstrate they could swim by completing a length of the pool. It did not matter how old they were, how tall they were, or what they said about their abilities. Everyone completed the same assessment before they had pool privileges.
One day, two people showed up to take the test.
The first was a former Olympian. Beautiful swimmer — I knew it the moment they approached the water. They wanted to use the high dive. Rules are rules. The Olympian started a few feet from the pool edge, ran across the pool deck, dove in, swam the length with a stroke that looked effortless, climbed out.
The second was someone who had just finished a beginner swimming lesson series and was still unsure of the water. They carefully lowered themselves in from the wall, pushed off, and made it to the other side — slowly, using a lot of effort, but they got there.
Both passed the test.
But here is what stayed with me: the Olympian had ignored two clear signs posted at the pool — “No diving” and “No running on pool deck.” They were technically the stronger swimmer. But they posed a real safety risk. They nearly dove onto another swimmer. They had to be corrected and reminded of the rules before they could use the facility freely.
The new swimmer? They followed every rule. They were still developing their stroke. But they were safe. They were attentive. They were, in some meaningful way, a better member of the pool community.
Clinical competence and professionalism are separate developmental tracks.
A resident can have brilliant clinical instincts and still struggle with how they communicate under pressure, how they treat a nurse who catches their mistake, or whether they follow the institutional protocol even when they are confident they know better. A senior attending can be technically excellent and still be at the beginning of their development as a leader or mentor.
This is precisely why Milestones and Entrustable Professional Activities matter. And it is precisely why physician development cannot stop the moment training ends.
How Medical Education Caught Up: Milestones and Entrustable Professional Activities
For most of the twentieth century, medical training operated on a time-and-numbers model. Complete a three-year residency. Perform a certain number of procedures. Log the required clinical hours. Graduate, obtain licensure, and begin independent practice.
The assumption built into this model was that time plus exposure equals competence. We now know this is not reliably true.
Two frameworks have fundamentally changed how we think about physician training, and both are worth understanding — not just by program directors and trainees, but by every physician who wants to understand their own development.
The ACGME Milestone Project
The ACGME Milestone Project represents one of the most significant shifts in graduate medical education in the last twenty years. Beginning in earnest around 2013, the ACGME worked with specialty-specific review committees to develop milestone frameworks: descriptors of observable physician behaviors organized along a developmental continuum from novice to expert.
Milestones are organized around six core competencies established by the ACGME: Patient Care, Medical Knowledge, Practice-Based Learning and Improvement, Interpersonal and Communication Skills, Professionalism, and Systems-Based Practice.
The critical insight embedded in the Milestone framework is this: development is not binary. A resident is not either competent or incompetent. They are somewhere on a continuum — and the goal of training is to help them move along it through targeted feedback, deliberate practice, and increasing levels of responsibility.
This is andragogy made visible in graduate medical education. The Milestone framework asks educators to assess not just what a trainee knows, but where they are developmentally — and then to provide the specific support that moves them forward.
Entrustable Professional Activities
Where Milestones describe developmental competencies, Entrustable Professional Activities (EPAs) describe the work itself.
An EPA is a clinical task or responsibility that can be entrusted to a trainee once they have demonstrated sufficient competence. EPAs were first articulated by Olle ten Cate in 2005 and have been adopted broadly across medical education. The Association of American Medical Colleges developed thirteen Core EPAs for Entering Residency, and many specialties have developed their own EPA frameworks.
The entrustment decision — the judgment by a supervisor that a trainee can perform a specific clinical task with a specific level of independence — is one of the most consequential acts in medical education. It is also one of the most humanizing. Rather than asking “did the resident complete the required number of procedures?” we ask “is this person ready to do this independently? What have I actually observed? What has changed?”
This shift from counting to observing, from checking boxes to making professional judgments, mirrors the shift from a purely skills-based model of physician development to a growth-and-competency model.
For a deeper dive on how these frameworks apply to career-stage transitions: What Every New Attending Physician Needs to Know and Transition to Residency.
The August Day I Understood the Cycle
Back to that hot August morning.
What nobody told me when I walked into that orientation room — sweating in my shorts and T-shirt, scanning faces for evidence that someone had made an administrative error — was that the cycle I was about to enter had a name. That it was predictable. That it would repeat.
Here is how it went.
In medical school, self-doubt was loudest. I did not know what I did not know, which meant I could not even calibrate my own ignorance. Gradually, I learned. And as I learned, I became more confident — not recklessly so, but meaningfully. By the end of medical school I knew I belonged.
Then residency started, and the doubt came back.
New environment. New expectations. Increased responsibility. The confidence I had earned as a fourth-year medical student was contextual — it applied to that version of the role, not this one. I was a beginner again in important ways, even while retaining everything I had learned.
Then fellowship. Then my first attending position. Each transition brought a version of that August morning back: the room I was not sure I deserved to be in, the voice asking whether I was truly ready.
What I have come to understand — and what I try to help every physician I coach understand — is that this cycle is not a malfunction. It is the mechanism of growth. The doubt signals that you are at a genuine edge. The growing confidence that follows is earned. And the competence you build at each stage does not disappear when the next stage begins — it becomes the foundation you stand on.
The problem comes when physicians are not taught to recognize the cycle. When the doubt arrives — mid-career, post-promotion, after a difficult case or a leadership role that felt too big — they interpret it as evidence of failure rather than evidence of growth. That misinterpretation is one of the most common things I work through with coaching clients.
The Developing Doctor Evolution Ladder™
Everything above — the adult learning theory, the swimmer story, the Milestone framework, the August morning — converges in a framework I developed to map the full arc of a physician’s career: the Developing Doctor Evolution Ladder™.
The Evolution Ladder is not a description of titles or credentials. It is a map of the central developmental question a physician is living at each stage of their career. Those questions change as you grow. The ladder captures that movement.
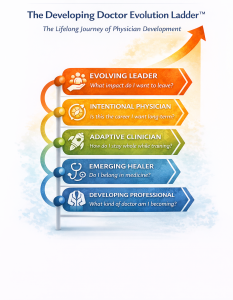
The Five Stages
Stage 1: Developing Professional What kind of doctor am I becoming?
This is the stage of formation. Medical school, early clinical exposure, the first real encounters with patients, death, failure, and the gap between who you hoped to be and the complexity of what medicine actually asks of you. The central work here is identity: not just learning clinical skills, but beginning to understand what kind of physician you are becoming and why.
The imposter syndrome is loudest at this stage — which makes sense, because the identity is still being built. You are not yet sure who you are in this role. That uncertainty is not a problem to solve. It is the developmental work itself.
Stage 2: Emerging Healer Do I belong in medicine?
Residency and early fellowship. You have crossed the threshold into real clinical responsibility. The training wheels are partially off. You are developing genuine competence, and with it, a cautious, growing sense of belonging. But belonging is not yet settled. A difficult case, a critical supervisor, a personal crisis — any of these can send the question back to the surface.
This is the stage where mentorship matters most, where early coaching has its highest leverage, and where the habits that will either protect or erode a long career are first formed.
Stage 3: Adaptive Clinician How do I stay whole while training?
This is the stage most physicians spend the longest time in — attending physician life, often extending through the first decade or more of practice. You are clinically competent. You belong. But the demands of the system are pressing against you, and the question is no longer whether you can do the work. It is whether you can sustain the work without disappearing into it.
This is the stage where burnout most commonly arrives. It is also the stage where coaching is most commonly sought — because the tools that got you here are no longer enough to carry you forward. The developing swimmer is following the rules; the Olympian has stopped paying attention to them. At this stage, the most important growth is not clinical. It is human.
Stage 4: Intentional Physician Is this the career I want long-term?
A physician at this stage has built clinical mastery, survived the system’s early pressures, and arrived at a more deliberate relationship with their own career. The question is no longer about survival or belonging. It is about choice. Is this what I actually want? Am I practicing the way I believe medicine should be practiced? What would I change if I could?
This is the Mezirow stage — the transformative learning phase where assumptions get examined. Physicians here often make the most significant career redesigns: reducing clinical time, taking on leadership, exploring nonclinical work, founding something new. Not because they are fleeing medicine, but because they are finally choosing it intentionally.
Stage 5: Evolving Leader What impact do I want to leave?
The final and ongoing stage — not a destination but a disposition. The physician at this stage has moved from asking what medicine can give them to asking what they can give medicine. They are developing others. Shaping institutions. Contributing knowledge, mentorship, and leadership to the profession they have spent a career building.
The August doubt still visits occasionally. But it has been transformed from a threat into a companion — evidence that the work still matters, that the edges of growth are still being approached.
The arrow on the Evolution Ladder points upward and outward — because this is not a closed loop. Development at its best is generative. What you build, you pass on.
Where Are You on the Ladder?
Most physicians, when they first encounter the Evolution Ladder, immediately know which stage resonates. Some feel the pull of two adjacent stages simultaneously — which usually means they are in transition. A few realize they have been operating at one stage while the circumstances of their career have moved them into another, which explains why something feels off.
The ladder is not a ranking. Stage 5 is not better than Stage 1. Each stage has its own dignity, its own developmental tasks, its own version of what thriving looks like. The goal is not to reach the top as fast as possible. The goal is to be fully present to the stage you are actually in.
The Developing Doctor Operating System™: How Coaching Actually Works
The Evolution Ladder tells you where you are. The Developing Doctor Operating System™ is how we move you forward.
These are two distinct frameworks, and the distinction matters. The Ladder is diagnostic — it helps you locate yourself on the developmental map. The Operating System is the coaching methodology — the structured process I use to help physicians create lasting change at any stage on that ladder. At the center of the OS is a single goal: to help every physician thrive in medicine.
The Operating System moves through four phases:
Identify — Know Yourself
Before anything else, you need a clearer picture of who you are: your values, your strengths, your patterns, and the assumptions that are shaping your choices without your full awareness. Most physicians arrive at coaching with a presenting problem — burnout, career uncertainty, a difficult relationship, a leadership challenge. The Identify phase helps us understand what is actually driving it. We use tools like values clarification, character strengths assessments, and the Maslach Burnout Inventory to build an honest baseline. You cannot navigate toward something better if you do not know where you are starting from.
Align — Choose Your Path
Once you know yourself more clearly, the next question is whether your current path reflects that knowledge. Align is about making choices that are congruent — with your values, your strengths, your season of life, and what you actually want medicine to feel like. This is where many physicians experience the shift from survival mode to intentional design. It is also where the Mezirow-style assumption examination happens: not just “what should I do?” but “why have I been doing what I have been doing — and does it still make sense?”
Develop — Build Your Skills
Clarity is not enough. You also need capability. The Develop phase is where we build the specific nonclinical skills that medicine rarely teaches: setting and holding boundaries, having difficult conversations with composure, communicating across different personality styles, leading teams without burning through the people on them, managing time in a way that respects your values, and navigating the institutional landscape strategically rather than reactively. This is Kolb in action — structured experimentation, feedback, reflection, and iteration.
Sustain — Create Your Future
Change that does not stick is not change. The Sustain phase is about building the habits, systems, and support structures that make the growth durable. What will you do when the old patterns resurface? Will they resurface? What accountability structures will keep you moving? What practices of ordinary joy, reflection, and self-awareness will you protect? The goal here is not just to solve the immediate problem but to build the infrastructure for a lifelong career in medicine that continues to grow, adapt, and satisfy.
The outcome of moving through the Operating System is not a single answer. It is three things: clarity about who you are and what you want, capability to create the career and life you are designing, and awareness of the impact you are capable of having — on patients, on colleagues, on the profession, and on the people who will come after you.
The Ladder and the OS work together this way: the Ladder tells you which developmental questions are most alive for you right now. The Operating System provides the structured process for answering them. A Developing Professional working on identity formation uses the OS differently than an Intentional Physician reconsidering their career direction — but both move through Identify, Align, Develop, and Sustain. The framework is stage-agnostic. The application is always personal.
The work of coaching at The Developing Doctor draws on all of this:
- Andragogy: respecting that you are a self-directed adult who brings decades of experience and needs to find your own answers — not be handed someone else’s
- Transformative learning: creating conditions for the assumption-examination that produces genuine shifts in how you see your career and yourself
- Experiential learning: using structured reflection to extract meaning from what you have already lived through
- Milestones and EPAs: applying a developmental rather than a binary lens to where you are and where you are going
- The Evolution Ladder: providing the developmental map that tells you which questions matter most right now
- The Operating System: providing the coaching methodology that helps you answer those questions and create durable change
Physician coaching vs. therapy — and how to know which you need
Why physician coaching is the tool you need
Coaching for physicians: sustainable clinical medicine
The Imposter Syndrome That Never Fully Leaves
I want to return to that August morning one more time — because there is something important I left out.
The self-doubt I felt walking into orientation was not unique to medical school. I felt it again when I started residency. Again when I began fellowship. Again when I became a junior attending, when I was named fellowship director, when I was appointed to lead a learning community, when I became a division chief.
Each time, I thought:
This is the one where they find out.
What changed — gradually, over years, through mentorship and coaching and deliberate reflection — was not that the voice went quiet. It was that I learned to hear it differently. The self-doubt stopped being a verdict and became a signal. A signal that I was at a genuine growth edge. That I was in exactly the right place for development to happen.
Somewhere around mid-career, the self-doubt became loud enough that I could not manage it alone anymore. The tools that had served me were not enough. That is what led me to coaching — not as a patient, not as a student, but as a person who needed a structured space to think clearly about who I was becoming and what I wanted my career to be.
That experience, the mid-career reckoning, the coaching relationship that followed, and the insight it produced, is what The Developing Doctor was built on.
If you are in that place right now, accomplished, capable, and quietly wondering whether you are still in the right place, this is for you.
For the related post on imposter syndrome across career stages: Overcoming Imposter Syndrome as a Doctor: Reclaim Your Confidence.
Hub: All Physician Development Posts
This cornerstone page links to the full collection of physician development content on The Developing Doctor.
Career Stage Transitions
- What Every New Attending Physician Needs to Know
- Transition to Residency: What No One Tells You
- Advice for Residents: Thriving in the Middle of Training
- Physician Leadership Coaching for Academic Doctors
Identity and Self-Awareness
- Overcoming Imposter Syndrome as a Doctor
- Physician Core Values and Value Misalignment
- Character Strengths: What Are You Really Good At?
- Emotional Intelligence for Physicians
Growth Without Burnout
- Growth Without Burnout in Healthcare
- Physician Development Doesn’t Stop After Training
- Three Steps to Planning a Medical Career
Medical Education
- Navigating Medical School Challenges
- How to Become a Doctor: A Comprehensive Guide
- Study Strategies That Actually Work in Medical School
Coaching and Mentorship
- Why Physician Coaching Is the Tool You Need
- Physician Leadership & Mentorship
- Coach, Therapist, Mentor, or Advisor? Understanding the Difference
Cornerstone Hubs
- Physician Burnout, Moral Injury & Ordinary Joy
- Physician Career Growth & Nonclinical Paths
- Physician Leadership & Mentorship
Video and Audio Resources
YouTube
- The Developing Doctor YouTube Channel
- Watch: Leadership Skills for Doctors: How to Build Influence in Healthcare
- Watch: Finding and Being a Mentor in Medicine
- Watch: How Coaching Transformed My Physician Career
- Watch: How to Make Charting 15 Minutes Faster Using Marginal Gains
Podcast
- The Developing Doctor Podcast — episodes on physician development, coaching, and sustainable careers in medicine
Key External References
- ACGME Milestone Project: acgme.org/milestones — the foundational framework for competency-based graduate medical education
- Entrustable Professional Activities (EPAs): AAMC Core EPAs for Entering Residency — thirteen EPAs that define the work of a first-year resident
- Ten Cate O. Entrustability of professional activities and competency-based training. Med Educ. 2005;39(12):1176-1177. — original articulation of the EPA concept
- Knowles MS, Holton EF, Swanson RA. The Adult Learner: The Definitive Classic in Adult Education and Human Resource Development. 8th ed. Routledge; 2015. — foundational text on andragogy
- Mezirow J. Transformative dimensions of adult learning. Jossey-Bass; 1991. — framework for perspective transformation in adult development
- Kolb DA. Experiential Learning: Experience as the Source of Learning and Development. Prentice-Hall; 1984. — the experiential learning cycle
- International Coaching Federation: coachingfederation.org — standards and ethics for professional coaching
- Lucey CR. Medical education: Part of the problem and part of the solution. JAMA Intern Med. 2013;173(17):1639-1643. — on the limits of traditional medical training
- Densen P. Challenges and opportunities facing medical education. Trans Am Clin Climatol Assoc. 2011;122:48-58. — on the pace of medical knowledge growth and implications for training
Frequently Asked Questions
What is the Developing Doctor Evolution Ladder™?
The Evolution Ladder™ is a physician career development framework created by Dr. Ben Reinking that maps the lifelong journey of a physician’s growth through five named stages, each anchored by a central developmental question: Developing Professional (What kind of doctor am I becoming?), Emerging Healer (Do I belong in medicine?), Adaptive Clinician (How do I stay whole while training?), Intentional Physician (Is this the career I want long-term?), and Evolving Leader (What impact do I want to leave?). The Ladder draws on adult learning theory, competency-based medical education, and two decades of clinical and coaching experience to give physicians a map for where they are — and what the work of this stage actually requires.
What is the Developing Doctor Operating System™?
The Operating System™ is the coaching methodology Dr. Ben Reinking uses to help physicians create lasting change at any stage of the Evolution Ladder. It moves through four phases — Identify (Know Yourself), Align (Choose Your Path), Develop (Build Your Skills), and Sustain (Create Your Future) — with Thrive in Medicine at the center. The goal of every coaching engagement is that a physician leaves with three things: clarity about who they are and what they want, capability to build the career they are designing, and awareness of the impact they are capable of having.
What is the difference between the Evolution Ladder and the Operating System?
The Ladder is diagnostic — it helps you locate yourself on the developmental map and understand which questions are most alive for you right now. The Operating System is the coaching process — the structured methodology for answering those questions and creating durable change. Think of it this way: the Ladder tells you where you are on the journey; the Operating System is how we move forward together. A physician at any stage of the Ladder — from Developing Professional to Evolving Leader — can benefit from moving through the Operating System.
What are Entrustable Professional Activities and why do they matter?
Entrustable Professional Activities (EPAs) are specific clinical tasks or responsibilities that training programs use to assess whether a trainee is ready to perform them independently. Rather than tracking numbers of procedures or time in training, EPAs focus on observed competence: has this person demonstrated, in real clinical situations, that they can be trusted to do this work safely? The EPA framework was developed by Olle ten Cate in 2005 and adopted broadly in medical education because it aligns with how expertise actually develops — through supervised practice, feedback, and increasing entrustment. Understanding EPAs also illuminates how the Evolution Ladder’s five stages map to the real structure of physician development: each stage shift represents a change in the level of entrustment a physician holds.
Is physician development the same as continuing medical education (CME)?
CME addresses clinical knowledge currency — staying current with evolving evidence and guidelines. Physician development is broader. It encompasses clinical competence but also professional identity, leadership capacity, communication skills, emotional intelligence, career design, and the psychological dimensions of a long career in medicine. CME keeps your knowledge current. Physician development keeps you growing as a whole person within your profession.
How does coaching fit into physician development?
Coaching provides the structured reflection that physician development requires but that busy clinical careers rarely make space for. Through the Developing Doctor Operating System, a coach helps you identify where you are on the Evolution Ladder honestly, understand what is holding you at a particular stage, build the specific skills that will move you forward, and navigate the psychological dimensions of career transitions — including the imposter syndrome that recurs at every new threshold. Coaching is not remediation. It is what elite performers in every field use to sustain growth over the long arc of a career.
Does the self-doubt ever stop?
Not entirely — and that is actually a good sign. The self-doubt that accompanies every new developmental stage is evidence that you are taking your responsibilities seriously. What changes with experience, coaching, and deliberate reflection is your relationship to it. Rather than interpreting doubt as a verdict on your worthiness, you learn to recognize it as a signal that you are at a genuine growth edge. The cycle recurs throughout a career. Understanding that it is a cycle — not a character flaw — is one of the most liberating insights in physician development.
Ready to Take the Next Step?
Physician development is not something that happens to you. It is something you participate in actively — with the right framework, the right support, and the courage to keep growing even when the next stage feels unfamiliar.
If you are ready to work through where you are and where you want to go, I would be glad to talk.
Or explore the Mastery & Wellness: How to Thrive as a Physician course — a self-paced program built around the core skills that sustain a long, purposeful career in medicine.
About the Author Dr. Ben Reinking is a practicing pediatric cardiologist, certified physician development coach, and founder of The Developing Doctor. He has served as a fellowship program director. Other roles: medical school learning community director, and division chief at the University of Iowa. Dr. Ben lived the Evolution Ladder he teaches. He holds Master Coach certification through the International Coaching Federation and has coached hundreds of physicians across every career stage. He started swimming at age six, taught lessons through medical school, and still thinks the pool is one of the best places to understand how human beings actually develop.
Learn more at thedevelopingdoctor.com or connect on YouTube.