Physician Development Doesn’t Stop After Training
Medicine teaches us how to care for patients. We also need to learn how to care for ourselves.
As a pediatrician, I am trained to monitor development. At well visits, we assess growth and milestones. We ask about speech, motor development, social engagement, and cognitive progress. When something is not progressing as expected, support is provided. We connect families with speech therapists, occupational therapists, or developmental pediatricians who can help their child reach their potential.
The goal of these well visits is to identify issues early so that our patients thrive in all aspects of life.
Over the years, I have learned something equally important. The most powerful part of this process is not fixing problems — it is recognizing what is right and nurturing strengths. When we see a child who loves music, drawing, building, or storytelling, we encourage that curiosity. We help them develop the talents that come naturally. Well visits are not about fixing deficits. They are about cultivating potential.
Somewhere along the way, physicians lose sight of what is right about themselves. Years of tests, evaluations, and performance metrics have conditioned us to focus on where we fall short. To focus on what is wrong. To ignore what is right.
The direct answer: Physician development does not end at residency graduation — it continues throughout an entire career. The physicians who thrive long-term are not the ones who work hardest after training ends. They are the ones who continue to grow: building self-awareness, developing nonclinical skills, and intentionally designing careers that remain meaningful as they evolve.
The Myth of the Finished Physician
Medical training often carries an implicit assumption: once we complete residency, the major milestones of professional development have been met. We graduate. We become attendings. And from that point forward, the expectation is simple — be competent, produce, put your head down and work hard.
But the growth does not stop when training ends. If anything, the challenges of practicing medicine demand moredevelopment, not less.
Physicians lead teams, navigate complex systems, communicate in emotionally difficult situations, and sustain demanding careers over decades. Yet most of us were never formally taught how to continue developing outside of structured training. So physicians do what physicians have always done: we adapt on our own. Sometimes we succeed. Sometimes we struggle. Often, we quietly wonder whether the way medicine is practiced today is sustainable.
Physicians are not finished products at graduation. They are still developing.
Physicians Are Still Developing
The physicians who reach out to me for coaching are rarely people who are failing. They are often highly capable people who care deeply about their work. What they share is something different — they feel stuck, frustrated, or misaligned. They want to keep practicing medicine, but sense that something about the way they are working, or the way medicine is structured, no longer fits.
What they are experiencing is not a personal failure. It is a developmental moment.
Just as children move through stages of growth, physicians evolve through stages of professional development. Recognizing which stage you are in — and what that stage requires — changes everything.
The Physician Development Ladder
Over time, I have come to see the physician journey through a developmental lens. I call this the Physician Development Ladder. At different points in a medical career, physicians face different questions, different challenges, and different growth opportunities. Each stage requires new skills, new self-awareness, and new ways of thinking about work.
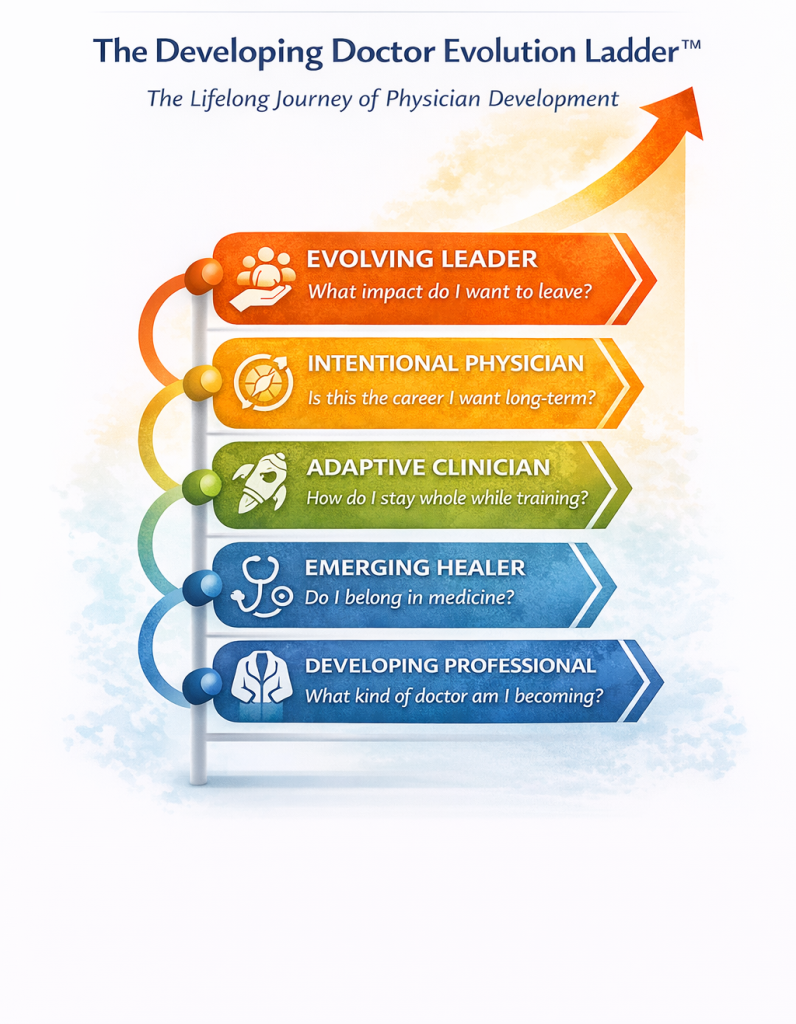
The five stages are:
- Emerging Healer — Exploring belonging and purpose; navigating the transition into medicine’s culture and identity
- Developing Professional — Forming a coherent professional identity; learning the rules of clinical practice
- Adaptive Clinician — Learning to thrive under sustained pressure; building resilience and efficiency
- Intentional Physician — Redefining success and alignment; reconnecting work to values after years of practice
- Evolving Leader — Expanding influence and legacy; shaping systems, teams, and the next generation
Medicine rarely provides structured guidance for navigating these stages after postgraduate training ends. Instead, many physicians are left to figure it out alone — or to stall at a stage that no longer serves them.
The Developing Doctor Operating System
If development continues throughout a physician’s career, the natural question becomes: how do we support it intentionally?
This is where the Developing Doctor Operating System comes in — a framework for purposeful professional growth across every stage:

- Identify — Understand your values, strengths, and motivations. Know what drives you and what depletes you.
- Align — Ensure your work and decisions reflect what matters most to you. Close the gap between your values and your daily reality.
- Develop — Build the nonclinical skills that determine long-term success — including leadership, communication, and emotional intelligence.
- Sustain — Create a career structure that allows you to keep practicing medicine without losing your sense of purpose, your health, or the people you love.
These steps are not linear. They repeat throughout a physician’s career. Each time we revisit them, we gain deeper clarity about who we are and how we want to practice.
Development is not a one-time event. It is a professional practice.
What If We Treated Physician Development Like Pediatric Development?
In pediatrics, we recognize that development takes time. We expect children to grow, learn, and change. We intervene when they need support — but we also celebrate their emerging strengths and meet them where they are developmentally.
Imagine if we approached physician development the same way.
Instead of assuming that doctors should simply endure the system, we would recognize that they are evolving professionals who benefit from reflection, guidance, and intentional growth. We would encourage physicians to develop their strengths, not just correct their deficits. And we would recognize that supporting physician development is not just good for doctors — it is good for patients, teams, and the healthcare system as a whole.
Physician Development Never Stops
Children grow into adults. Adults may no longer grow taller — but they continue to develop throughout their lives. Physicians are no exception.
The doctors who thrive over the long term are not the ones who work the hardest after training ends. They are the ones who continue to evolve — who build self-awareness, invest in the skills their training overlooked, and design careers that remain meaningful as they change.
Medicine teaches us how to care for patients and nurture their potential. We also need to learn how to develop ourselves. That work never really ends.
Ready to develop more intentionally? If you are feeling stuck, misaligned, or ready for a more sustainable path forward in medicine, coaching can help you gain clarity, strengthen your leadership, and build a career that fits who you are now. Explore coaching through The Developing Doctor →
Frequently Asked Questions
Does physician development really continue after residency?
Yes — and significantly. Residency trains clinical competence. What comes after — leading teams, navigating institutional complexity, sustaining a decades-long career, finding meaning through change — requires a different kind of growth that formal training rarely addresses. The physicians who thrive long-term invest in this development deliberately rather than leaving it to chance.
What is the Physician Development Ladder?
The Physician Development Ladder is a framework developed at The Developing Doctor that describes five stages of professional growth in medicine: Emerging Healer, Developing Professional, Adaptive Clinician, Intentional Physician, and Evolving Leader. Each stage involves distinct developmental challenges and requires different skills, mindsets, and kinds of support. Recognizing your current stage helps you understand what growth actually looks like for you right now.
What nonclinical skills do physicians most need to develop?
The most commonly underdeveloped nonclinical skills in physicians include: emotional intelligence, boundary-setting and communication under stress, leadership and team management, negotiation, and self-awareness. These skills determine long-term career sustainability and satisfaction more than clinical expertise does — yet medical training rarely addresses them directly.
What is the Developing Doctor Operating System?
The Developing Doctor Operating System is a four-stage framework for intentional physician growth: Identify (understand your values, strengths, and motivations), Align (ensure your work reflects what matters to you), Develop (build the nonclinical skills that sustain a career), and Sustain (create structures that protect your capacity over time). It is designed to be revisited at each stage of a physician’s career as needs and circumstances evolve.
How can coaching support physician development?
Physician coaching provides structured, personalized support for the developmental challenges that medicine leaves unaddressed. A coach helps you identify where you are in your professional development, what is holding you back, and what skills and changes will move you forward most effectively. Unlike mentorship, which draws on someone else’s experience, coaching is centered on your specific context, goals, and values.
About the Author Dr. Ben Reinking is a practicing pediatric cardiologist, certified physician coach, and founder of The Developing Doctor. With nearly two decades of clinical experience and roles as fellowship director and division director at the University of Iowa, Ben created the Physician Development Ladder and Developing Doctor Operating System to help physicians grow intentionally at every stage of their careers. Learn more at thedevelopingdoctor.com.
Updated April 2026





