The Physician Development Ladder: Preparing Doctors for a Changing World
Author’s Note: As a pediatric cardiologist, a medical educator, and a coach, I’ve sat on every side of the table. I’ve interviewed anxious premeds, shepherded fellows through subspecialty training, served on promotion committees, and now lead an academic division. I’m also a learning-community director who welcomes medical students on their first day of orientation and later helps write their Medical Student Performance Evaluations as they prepare for residency applications. And through my private coaching practice, I’ve walked alongside physicians at every stage of their careers.
Across these roles one truth keeps surfacing: our people are our greatest asset. No policy, technology, or workflow will fix healthcare unless we invest in the people who deliver the care. That’s why I’ve built my coaching around two complementary frameworks—the Physician Development Ladder and the Developing Doctor Operating System. Together they provide a roadmap and an engine for growth. In this post, I want to show you what those frameworks look like, why they matter, and how coaching can help physicians climb each rung of the ladder.
Why a Ladder? A Story From the Admissions Committee
I still remember interviewing a bright college senior for medical school. She spoke passionately about global health and told me she wanted to become the kind of doctor who makes a difference. A few months later, as an orientation leader, I recognized her face—wide-eyed and nervous on the first day of medical school. Years after that, as fellowship program director, I heard her voice crack with exhaustion and doubt during a conversation about whether to pursue advanced subspecialty training. Later, on the faculty promotion committee, her name crossed my desk again as we reviewed her academic dossier.
Those moments stayed with me because they reveal something important: physicians do not develop in a straight line. We evolve. We revisit old questions in new contexts; we gain skill, lose confidence, find purpose, hit walls, and start again. The farther I’ve moved in my own career—from admissions committee member to fellowship program director to division director—the more convinced I’ve become that physician development is not a series of isolated checkpoints. It is a lifelong process.
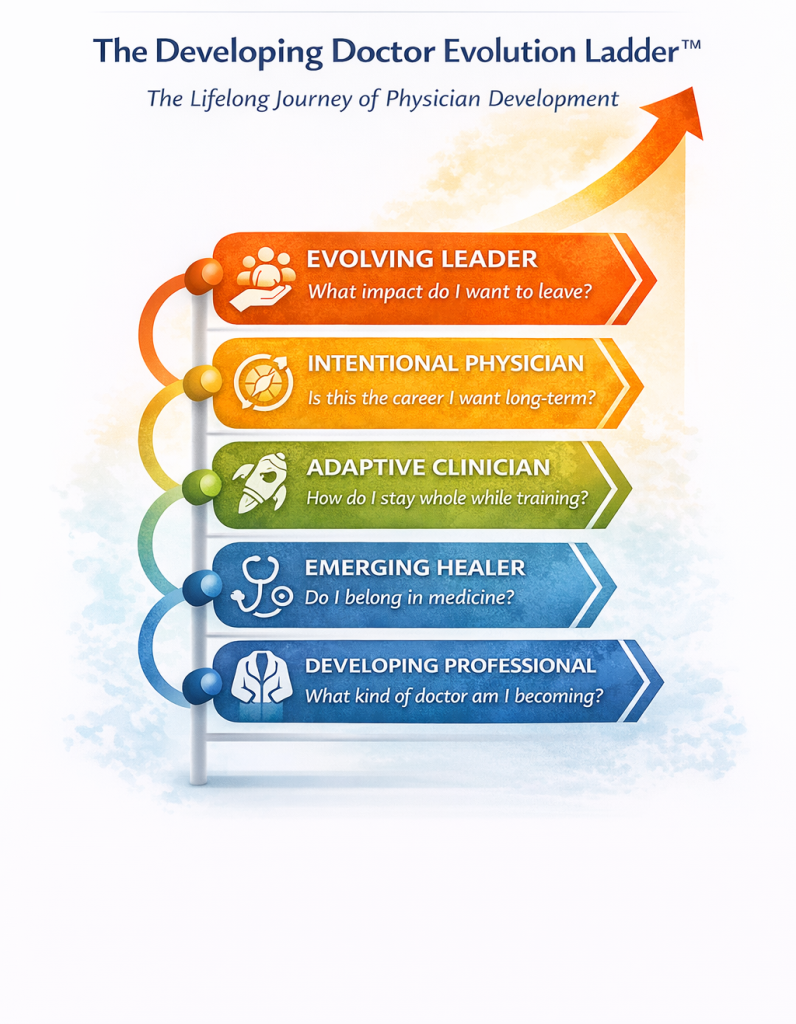
To capture that reality, I developed the Physician Development Ladder. It names five stages of growth, each paired with a question physicians commonly ask as they move through training, practice, and leadership:
- Developing Professional – What kind of doctor am I becoming?
- Emerging Healer – Do I belong in medicine?
- Adaptive Clinician – How do I stay whole while training?
- Intentional Physician – Is this the career I want long-term?
- Evolving Leader – What impact do I want to leave?
These are not rigid titles. They are developmental phases. A resident may wrestle with belonging. A mid-career attending may suddenly ask whether this is the career they want long-term. A division director may be asking what legacy matters now. The Ladder helps make sense of those shifts and reminds us that growth in medicine is cyclical, not linear.
The Operating System: Identify, Align, Develop, Sustain
If the Ladder maps the journey, the Developing Doctor Operating System powers the climb. It gives structure to the coaching process and turns reflection into action. The four phases are simple, but they are not shallow:
Know yourself.
Choose your path.
Build your skills.
Create your future.
Identify is where awareness begins. Physicians examine stress patterns, emotional triggers, strengths, and values. They ask what is really driving the dissatisfaction beneath the surface. Is it overwork? Misalignment? Loss of meaning? This is the part of development medical training often skips, even though it shapes everything that follows.
Align is where clarity becomes decision-making. Once physicians understand what matters most, they begin aligning daily choices, career direction, and boundaries with those values. This is often the stage where people realize they do not need to keep saying yes to everything simply because they can.
Develop is where new skills are built. Sometimes that means communication, emotional intelligence, leadership presence, or conflict navigation. Sometimes it means time management, career strategy, or learning how to work from strengths instead constantly trying to fix a perceived weakness. It is the phase where growth becomes practical.
Sustain is what keeps development from turning into another short-lived productivity project. It focuses on building a career and life that can hold up. This is where physicians reconnect with the reasons they entered medicine in the first place while also creating systems that protect joy, health, and purpose.

What the Evidence Says About Coaching
I believe deeply in story, but I also believe in evidence. Coaching should not be framed as vague encouragement or soft support without substance. The literature is growing, and it increasingly supports what many of us have seen firsthand.
A 2025 randomized clinical trial published in Journal of General Internal Medicine found that physicians who participated in professional coaching experienced meaningful reductions in burnout. In that trial, small-group coaching participants had a 29.6% absolute reduction in burnout compared with an increase in burnout in the control group, suggesting that structured coaching may be both effective and scalable for attending physicians.1
Broader reviews of physician coaching have also found that coaching improves well-being and reduces distress and burnout. One review highlighted growing evidence that coaching helps physicians and trainees build resilience, self-compassion, and professional fulfillment.2 Another physician leadership review described coaching as a process of equipping people with the tools, knowledge, and opportunities they need to become more effective, with benefits for well-being, performance, and leadership development.3
Why this matters: Medicine has long assumed that high achievers will simply figure development out on their own. But self-neglect is not a sustainable strategy. Coaching works precisely because it creates protected space for reflection, accountability, and growth.
Walking the Rungs: My Own Experience
When I look back, I can see my own career through the Ladder.
As a trainee, I was a Developing Professional, asking what kind of doctor I was becoming. In the middle of training, I often felt like an Emerging Healer, wondering whether I truly belonged. During long stretches of academic medicine, leadership, and family life, I found myself in the Adaptive Clinician stage, asking how to stay whole while carrying so much responsibility.
Later, as I took on larger leadership roles, I became the Intentional Physician, asking whether the way I was practicing and leading matched the career I wanted long-term. And now, sitting in the division director chair, I increasingly feel the pull of the final rung: the Evolving Leader. What impact do I want to leave? How do I help build a culture where other physicians can thrive, not just survive?
That question has changed how I coach and how I lead. My experiences on admissions committees, as a fellowship program director, on faculty promotion committees, and as a learning-community director have shown me the same thing over and over again: if we want better doctors, better teams, and better healthcare, we have to invest in development long before someone is in crisis.
Why This Matters for Medical Education
Traditional medical education is excellent at teaching knowledge and testing performance. It is far less consistent at supporting identity formation, reflective growth, and sustainable professional development. We ask learners to become physicians, but we do not always give them language for the developmental work that transformation requires.
That gap shows up everywhere. It shows up in the student who wonders whether one difficult rotation means they are not cut out for medicine. Or in the resident who is high-performing on paper but quietly exhausted. It shows up in the attending who has built an impressive career and still cannot answer whether it is the life they actually want. It shows up in the physician leader who has positional authority but no framework for developing people.
The Physician Development Ladder helps name those moments. The Operating System helps move through them. Together, they offer a model for longitudinal growth that complements, rather than replaces, competency-based assessment.
How This Builds on Earlier Conversations
This idea does not stand alone. It builds on themes I’ve explored before on this site: that physician coaching is often the missing piece in medical training, that coaching and therapy serve different purposes, and that doctors need more than clinical expertise to create sustainable, meaningful careers. In earlier posts, I’ve written about burnout, purpose, emotional intelligence, and career alignment. The Ladder brings those themes together into a developmental framework.
It also reflects what I’ve learned in coaching conversations with physicians across career stages. People rarely come saying, “I need a ladder.” They come saying, “I feel stuck,” “I’m not sure I belong,” “I don’t know if I can keep doing this,” or “I want my career to mean something more.” The Ladder simply helps us recognize where they are and what kind of support they need next.
If We Want to Fix Healthcare, We Have to Invest in People
Healthcare loves to chase system solutions. New workflows and dashboards. New technologies. More structures. Some of those matter. But none of them will be enough if we continue to underinvest in the development of the people doing the work.
I believe this more strongly now than ever: our people are our greatest asset. If we want to repair healthcare, we need to invest in physicians not only as producers of clinical work, but as developing human beings. That means supporting self-awareness, alignment, skill-building, resilience, and leadership across the full arc of a career.
The Physician Development Ladder is one way to make that investment visible. The Operating System is one way to make it actionable. Coaching is one way to make it personal.
And when we do that well, we do not just create more capable physicians. We create more grounded doctors, healthier teams, and more humane care.
Final Thought
Every physician is becoming someone. The question is whether that development is happening by accident or with intention.
If you are asking deeper questions about your career, your identity, your leadership, or your future, you are not behind. You are developing. The goal is not perfection. The goal is growth that lasts.
That is the work of the ladder. That is the work of coaching. And that is the work of building a better healthcare system by investing in our people.
Ready to reflect on where you are in your own development?
Coaching can help you identify what matters, align your path, develop the right skills, and build a career that is sustainable.
References
- Khalili J, Miotto K, Wang T, et al. Professional coaching to reduce physician burnout: a randomized clinical trial. J Gen Intern Med. Published online July 11, 2025. doi:10.1007/s11606-025-09653-w.
- Review summarized in: “What is Physician Coaching? The Evidence.” Joy in Family Medicine. Updated June 2024.
- Martin M, Heroman WM. The evidence and impact of coaching: focusing on physician leadership coaching for improved outcomes. Healthcare Administration Leadership & Management Journal. 2025;3(5):249-252.
About Dr. Ben Reinking: Dr. Ben Reinking is a pediatric cardiologist, medical educator, and physician coach. Through The Developing Doctor, he helps physicians and trainees build sustainable careers rooted in self-awareness, growth, and purpose.





