Part 2: Provider-Oriented Solutions – Building a Better Workplace for Clinicians
In the first article of this series, we explored how systemic dysfunction, high costs and poor health outcomes fuel burnout among the people who deliver care. Nearly half of physicians still report symptoms of burnout, and the numbers are similar or worse for nurses and other front-line staff. Addressing the crisis requires redesigning the environment in which clinicians work. Evidence points to several strategies from flexible scheduling and teamwork to innovative technology and peer support that can restore joy and purpose for healthcare professionals.
Understanding the provider’s challenge
- High turnover and emotional strain are widespread. According to the American Hospital Association (AHA) 2026 Workforce Scan, first-year nurse turnover reached 29.9%, much higher than the average RN turnover rate of 16.4%. Emotional stress is the top driver of resignations, and insufficient staffing increases turnover risk by 68%. Replacing a single bedside nurse costs hospitals approximately $61,000.
- Flexible scheduling and downtime matter. In surveys of hospital nurse leaders, giving staff the ability to take a day off when needed, offering flexible scheduling and providing professional development were among the most effective ways to boost morale. An AMN Healthcare 2025 survey of more than 12,000 nurses found that 81% say flexible schedules would improve working conditions and 55% strongly agree that flexible scheduling would help balance work and family life. Yet only 34% of nurses have access to self-scheduling options.
- Burnout affects clinicians beyond doctors and nurses. A JAMA Network Open study found burnout rates of 47.3% for physicians, 56% for nurses and 54.1% for other clinical staff; non-clinical staff (including administrators) also reported a burnout prevalence of 45.6%. This shows that solutions must address all members of the care team.
Evidence-based solutions to support providers
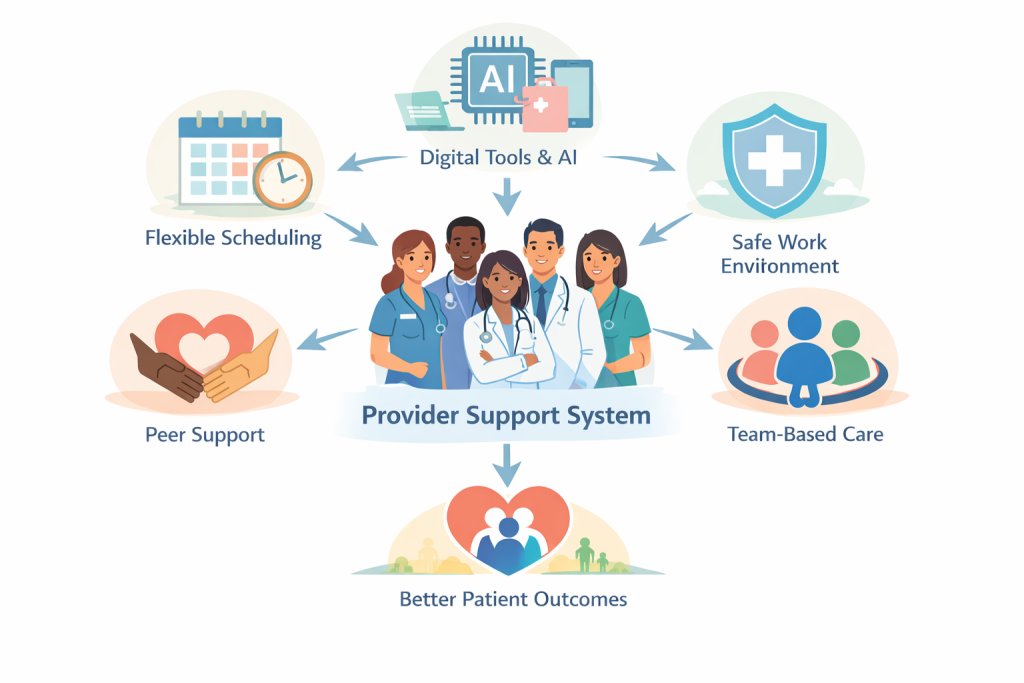
At-a-glance: a provider support system
The graphic below summarises the key pillars of a provider-centered ecosystem. A team of diverse clinicians is surrounded by five supports: digital tools & AI, a safe work environment, team-based care, peer support and flexible scheduling which collectively feed into better patient outcomes. Use this as a mental model for the initiatives described in the subsequent sections.
1. Reduce administrative burdens through smart technology
Clinicians spend enormous time on tasks that do not require medical expertise. Surveys by the American Medical Association (AMA) show that 57% of physicians believe the greatest value of artificial intelligence is reducing administrative burdens. Most doctors think AI could improve work efficiency, reduce stress and alleviate cognitive overload. In the same survey, 80% of physicians said AI would be most useful for documentation tasks (billing codes, charting), 72% for drafting discharge instructions, and 71% for automating prior-authorization requests.
Actionable steps
- Automate documentation and coding. Ambient AI scribes to clinician patient conversations and generate progress notes. Health systems such as Geisinger and Ochsner report that these tools save physicians about an hour per day.
- Streamline follow-ups and scheduling. The AHA workforce scan notes that many hospitals now pre-populate patient forms and automatically schedule follow-up visits so clinicians can spend more time with patients. Generative AI also drafts progress notes, summarises visit transcripts and updates medication lists.
- Engage front-line staff in technology decisions. Not every digital tool fits every environment; leaders must involve clinicians when implementing new tools and ensure that technology reduces, rather than shifts, administrative work.
2. Embrace team-based care and shared governance
Research from the National Academy of Medicine (NAM) shows that high-quality teamwork is associated with better clinician well-being and resilience. Studies have found that positive team culture and tight team structure correlate with lower clinician emotional exhaustion. Teamwork partially mitigates the relationship between heavy work demands and burnout and fully mitigates the link between job engagement and job satisfaction. Simply put, when clinicians feel psychologically safe, communicate effectively and share responsibility for outcomes, they are less likely to burn out.
Actionable steps
- Build multidisciplinary teams. Integrate physicians, nurses, pharmacists, social workers, advanced practice providers and allied health professionals. Ensure that each member practices to the full extent of training and shares a common purpose.
- Establish shared governance. Clinicians who participate in shared governance councils are less likely to experience burnout and more likely to remain with their employer. One study found that system-wide shared governance reduced new nurse turnover from 32.1% to 27.3%, saving about $2 million in recruitment, hiring and training costs.
- Invest in team-building and leadership training. Health systems should set measurable engagement goals, create environments where staff want to participate and develop leadership skills at all levels. Programs such as Northwestern Medicine’s “Scholars of Wellness†train clinicians in well-being science and change leadership; Ochsner Health appoints peer leaders to champion wellness.
3. Provide flexible scheduling and work-life balance
Flexible schedules give clinicians control over their time and reduce stress. In AMN Healthcare 2025 survey of nurses, 81% said flexible schedules would improve working conditions and 49% said flexible hours would encourage them to stay in the profession. The AONL Nursing Leadership Insight Study found that letting staff take a day off when needed, offering flexible scheduling and investing in professional development were among the most effective strategies to boost morale.
Actionable steps
- Implement self-scheduling and shift-trading platforms. Only a third of nurses currently have access to self-scheduling. Hospitals can adopt digital scheduling systems that let employees choose shifts within staffing parameters and swap shifts with colleagues.
- Offer hybrid or part-time roles. Some organizations are experimenting with hybrid arrangements and flexible schedules to address psychological well-being; these efforts have led to measurable improvements in perceived safety and emotional health.
- Respect personal time. Avoid mandatory overtime and ensure that time off is truly off. Leaders should model healthy boundaries.
4. Foster a culture of safety and belonging
Workplace violence is a major stressor for healthcare workers. Nearly 75% of the roughly 25,000 workplace assaults reported annually occur in healthcare settings, and the total financial cost of violence to hospitals in 2023 was about $18.27 billion. A safe environment is foundational for clinician well-being.
Actionable steps
- Enhance security and de-escalation training. Hospitals are deploying incident-reporting systems, staff duress alarms, weapons detection systems and de-escalation training. Main Line Health, for example, installed weapons detection, issued duress-signal badges and explored flexible schedules to address staff safety, leading to improved perceived safety and well-being.
- Promote belonging and peer recognition. Staff who feel respected and connected to a shared purpose are more likely to stay. Health systems recommend peer recognition programs, stay interviews and team-building events to strengthen community.
- Address discrimination and stigma. Removing intrusive behavioral-health questions from credentialing applications makes it easier for clinicians to seek care. As of May 2025, 635 hospitals and care facilities had removed these questions.
5. Expand peer support and mental health services
Peer support programs offer safe spaces for clinicians to discuss stress and learn coping strategies. Emory University’s EmBRACE peer support program trained more than 160 volunteers who conducted 1,387 sessions in 2024c50% more than in 2023. In a survey of peer supporters, 66% strongly agreed that the skills they gained made them more compassionate and supportive. Nationally, more than 73% of physicians agree that stigma surrounding mental health still exists, highlighting the need for confidential services.
Actionable steps
- Create confidential peer support networks. Programs like EmBRACE train volunteers to provide psychological first aid, with mechanisms to refer colleagues to professional counseling.
- Offer accessible mental health services. The Physicians Foundation’s 2025 survey reported that more than half of physicians experienced debilitating stress and anxiety, even though burnout levels declined. The Foundation urges stakeholders to reduce administrative burdens and provide stigma-free mental health access.
- Educate leaders to normalize help-seeking. Leadership must model vulnerability and encourage the use of wellness resources.
6. Support autonomy and professional growth
Researchers note that supportive leadership and autonomy giving clinicians a sense of choice in their work are vital for mitigating anxiety, depression and burnout. When physicians perceive that their opinions are valued, job satisfaction increases and burnout risk falls. Positive relationships with colleagues and opportunities for growth further buffer against burnout.
Actionable steps
- Solicit input on workflow and policy changes. Involve clinicians in designing new programs and selecting technology; use stay interviews and surveys to gauge needs.
- Invest in career development. Provide opportunities for continuing education, mentorship and leadership training. Programs like one on one coaching help providers develop confidence and peer connections.
- Recognize and reward excellence. Meaningful recognition and advancement opportunities signal respect and foster a sense of purpose.
Building a provider-centric program: where to start
Imagine building a new clinical program such as a specialized heart failure clinic with provider well-being as a core design principle. The following sequence reverses traditional priorities:
- Start with patients. Identify patient needs and design care pathways that minimise unnecessary steps. Use digital intake and telehealth to reduce travel and waiting time. Engage patients as partners in care decisions.
- Focus on providers. Determine the tasks, schedules and support clinicians need to deliver those services efficiently and joyfully. Build schedules that prioritise work-life balance, support team-based care, and ensure time for documentation and patient education. Provide mentoring, mental health resources and safe work environments.
- Allocate resources. Once patient and provider needs are defined, determine the physical capital (space, equipment) required. Examples include modular clinic rooms with telemedicine capabilities, quiet rooms for staff decompression and secure storage for equipment.
- Design the system. Create processes that coordinate patient flow, staffing, scheduling and data sharing. Use AI and automation to handle routine tasks and scheduling; embed peer support and training in orientation; implement shared governance; and adopt data-driven staffing models to maintain safe staffing ratios.
- Ensure financial sustainability. Finally, evaluate the program’s business model. Use value-based payment opportunities (e.g., chronic care management codes) and measure outcomes such as reduced turnover and improved clinician productivity. Demonstrate return on investment from lower turnover costs (nurse replacement cost of about $61k) and improved patient satisfaction.
Conclusion
Clinician burnout is not inevitable; it is a systems problem with clear, evidence-based solutions. By reducing administrative load through smart technology, fostering high-functioning teams, offering flexible scheduling, ensuring safety and belonging, expanding peer support and mental health services, and supporting autonomy and growth, healthcare organizations can rebuild the joy of medical practice. The result will not only be happier providers but also healthier patients and more sustainable health systems.
References
- American Hospital Association. (2026). Health care workforce: A system under pressure, poised for reinvention (2026 workforce scan). Chicago, IL: Author.
- AMN Healthcare. (2025). 2025 survey of registered nurses: A crisis in healthcare. Dallas, TX: Author.
- Mohr, D. C., Elnahal, S., Marks, M. L., & Derickson, R. (2025). Burnout trends among U.S. health care workers. JAMA Network Open, 8(4), e255954. https://doi.org/10.1001/jamanetworkopen.2025.5954
- American Medical Association. (2024). Physicians greatest use for AI? Cutting administrative burdens. Chicago, IL: Author.
- National Academy of Medicine. (2018). Implementing optimal team-based care to reduce clinician burnout. NAM Perspectives Discussion Paper. Washington, DC: National Academy of Medicine.
- Emory University School of Medicine. (2024). EmBRACE peer support program fosters compassion in health care.
- Physicians Foundation. (2025). 2025 survey of Americas physicians: Burnout, stress and stigma.
- Bakker, A. B., & Demerouti, E. (2007). The job demands–resources model: State of the art. Journal of Managerial Psychology, 22(3), 309 328.
- Cross Country Healthcare & Florida Atlantic University. (2025). Nurse career & satisfaction survey.



